Peripheral Arterial Disease
Peripheral Arterial Disease

What is Peripheral Arterial Disease?
Peripheral arterial disease (PAD) damages your arteries, which are blood vessels that deliver blood from the heart throughout the body. Peripheral arterial disease, which occurs in various forms, is present when the arteries to your arms or legs narrow or become clogged. This most often results from hardening of your arteries or atherosclerosis. In the lower extremities, ischemia can cause claudication (a term used to refer to impairment in walking, or pain, discomfort, numbness, or tiredness in the legs that occurs during walking or standing and is relieved by rest) in peripheral artery disease (PAD) or may cause critical limb ischemia (CLI) in severe cases.
The most common types of PAD include blood clots or atherosclerosis, a disease in which plaque, a sticky substance made up of fat, cholesterol, calcium, and other substances found in the blood, builds up inside your arteries. The plaque blocks blood flow and prevents oxygen from reaching tissue. This can cause pain, sores, or even dead tissue that can lead to strokes and heart attacks.
What are the symptoms of Peripheral Arterial Disease?
Some people experience pain or heaviness in their legs while walking, which prevents them from enjoying their lives. You may have PAD if you experience the following during activity:
- Aching, throbbing legs
- Pain and cramping
- Numbness
- Tingling
- Weakness
- Burning
- Discolored skin
You may be more likely to have PAD if (among other factors), you have high cholesterol, high blood pressure, diabetes or a history of smoking. An interventional radiologist can help determine if you have PAD through a simple test called an ankle brachial index test, or ABI, that compares the blood pressure in the upper and lower limbs or an examination using imaging techniques such as ultrasound, CT and MRI
How is Peripheral Arterial Disease Treated?
If lifestyle changes aren’t enough to treat your PAD, you might benefit from a minimally invasive interventional radiology treatment. In most cases, the doctor will make a small incision in your groin and, using X-rays or other imaging to guide him, thread a very thin catheter through your blood vessels to the blockage or narrowed artery. Depending on where the blockage is and how it looks, it may be treated in several ways including using drugs, balloons, and metal stents.
What can I expect after treatment?
Once the treatment is completed, the doctor removes the catheter and applies pressure to the tiny incision in your groin to allow it to heal. You will then lie flat on your back for several hours. Usually, you will be able to go home the same day, but there is a small chance you will be observed overnight and discharged in the morning. During a period of regular follow-up appointments, which can include ultrasound or other imaging tests, your doctor will monitor your progress after the therapy.
Critical Limb Ischemia?
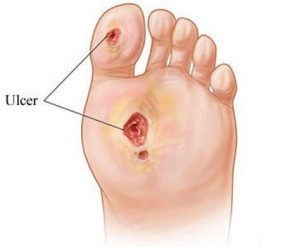
Ischemia is a serious condition in which there is inadequate blood flow and oxygen to a specific part of the body, generally caused by a narrowing or blockage of an artery. Critical limb ischemia, or CLI, is the severe version of PAD and results in the followings symptoms:
- severe pain (often at rest)
- tissue loss, such as a non-healing sore
- gangrene
Critical limb ischemia is serious and will not improve on its own. If the tissue of the limb has been affected; this requires immediate attention. An interventional radiologist will perform angiography help determine if revascularization (opening up) the blocked artery will help your condition. The poor prognosis demands a multidisciplinary approach involving interventional radiologists who are specialists in endovascular revascularization, surgeons, podiatrists, wound care experts, and other specialties to maximize patient outcomes.
You deserve to know all of your options. Contact your Primary Care Physician or GLMI directly for a consultation.




